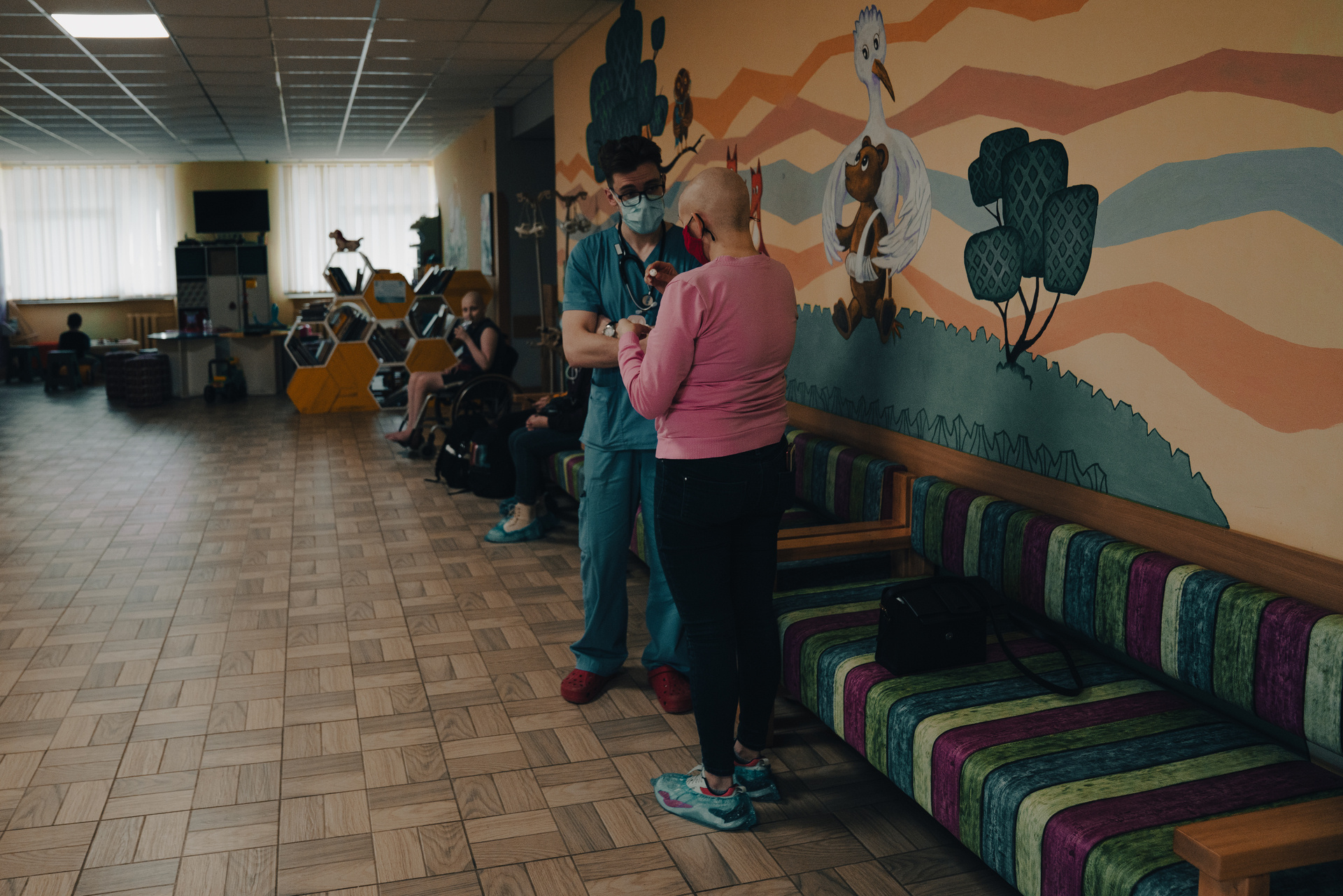When Dr Liliana Voloceai prescribed opioids to treat pain – or “narcotics” as they are widely called in the Republic of Moldova – to an older patient with advanced stage cervical cancer, the woman’s family viewed this as a sign that she was close to death. However, as time passed, the patient regained her strength and lived longer than all expectations. And that is not a miracle, says Liliana – that is how quality palliative care should work.
Overcoming fear: a major challenge for the doctor
Fear of the use of opioid medicines (opiophobia) is considered a serious barrier to the treatment of pain in many countries of the WHO European Region. This is also the case in the Republic of Moldova, where Liliana, originally an oncological surgeon, now works as a district oncologist and a palliative care specialist at the same hospital.
Liliana started working with palliative care patients during the COVID-19 pandemic. Even though she is an oncologist, Liliana says that it took her a while to feel confident when prescribing strong opioids. That is a challenge for any doctor who begins working in this field, she says.
“Pain triggers a primal fear in all of us. But for patients grappling with constant pain, the anxiety doesn't end there. They can also develop anxieties around changes to their established pain relief medications, even when such changes are intended to optimize their treatment,” adds Liliana.
She is one of the health professionals who received training in palliative care in the Republic of Moldova based on WHO-recommended practices. She thinks that the emotional component is the most delicate element when it comes to effectively treating pain.
“Doctors need to be very careful when proposing opioid medicines to patients. The stigma attached to these drugs can trigger fear and apprehension in both patients and doctors. So, for those just starting to master opioid use, the process can provoke anxiety,” adds Liliana.
Clear benefits of strong opioids
Strong opioids often evoke fear and negative associations, and these are hard to overcome – even with the clear evidence that opioid medicines are safe to use and work efficiently. When used correctly, strong opioids not only help to manage pain and other troublesome symptoms, evidence suggests that they are less addictive than tobacco or sleeping pills. Studies show that strong opioids do not shorten life and continue to effectively treat pain even when used for a long time.
That is exactly what happened to Liliana’s patient. When the woman began to take the right medicine at the right time and the right dose, the pain was relieved. Her appetite returned, she began to sleep well and her quality of life improved.
Pain should be treated – always
For Liliana, this story clearly demonstrates the power of palliative care. This approach is patient-centered and focuses first on well-being, and on improving the quality of life for people facing life-threatening conditions.
“Palliative care is an active approach to care and aims to improve the quality of life of patients, their family and caregivers. Palliative care is not about death but living well until you die, it can and should be provided along with curative treatment,” says Dr Julie Ling, Chief Executive Officer of the European Association of Palliative Care.
“Palliative care is not just for people with cancer. It addresses suffering from any serious health problem. Looking at the patient as a whole, palliative care addresses symptoms whether physical, psychological, social or spiritual.”
Palliative care in the Republic of Moldova is developing but there is still much unmet need. Despite the first cancer pain treatment protocol being implemented in 2010, access to and use of opioids is still very limited. Many health professionals remain concerned about their use.
“For me personally, the hardest part was to begin using opioid-based patches. They effectively treat pain, but they work in a totally different manner from the injections that have been used in Moldova for many years,” says Liliana. “I am grateful to the patients for the trust that they have shown in my knowledge and experience with prescribing strong opioids for their pain. It is very satisfying to see their pain well controlled as this means that they have better quality of life.”